Stop Claim Denials Before They Start
Pre-submission claim analysis that catches denial risks, validates coding accuracy, and ensures documentation completeness.
All for just
17 cents per claim
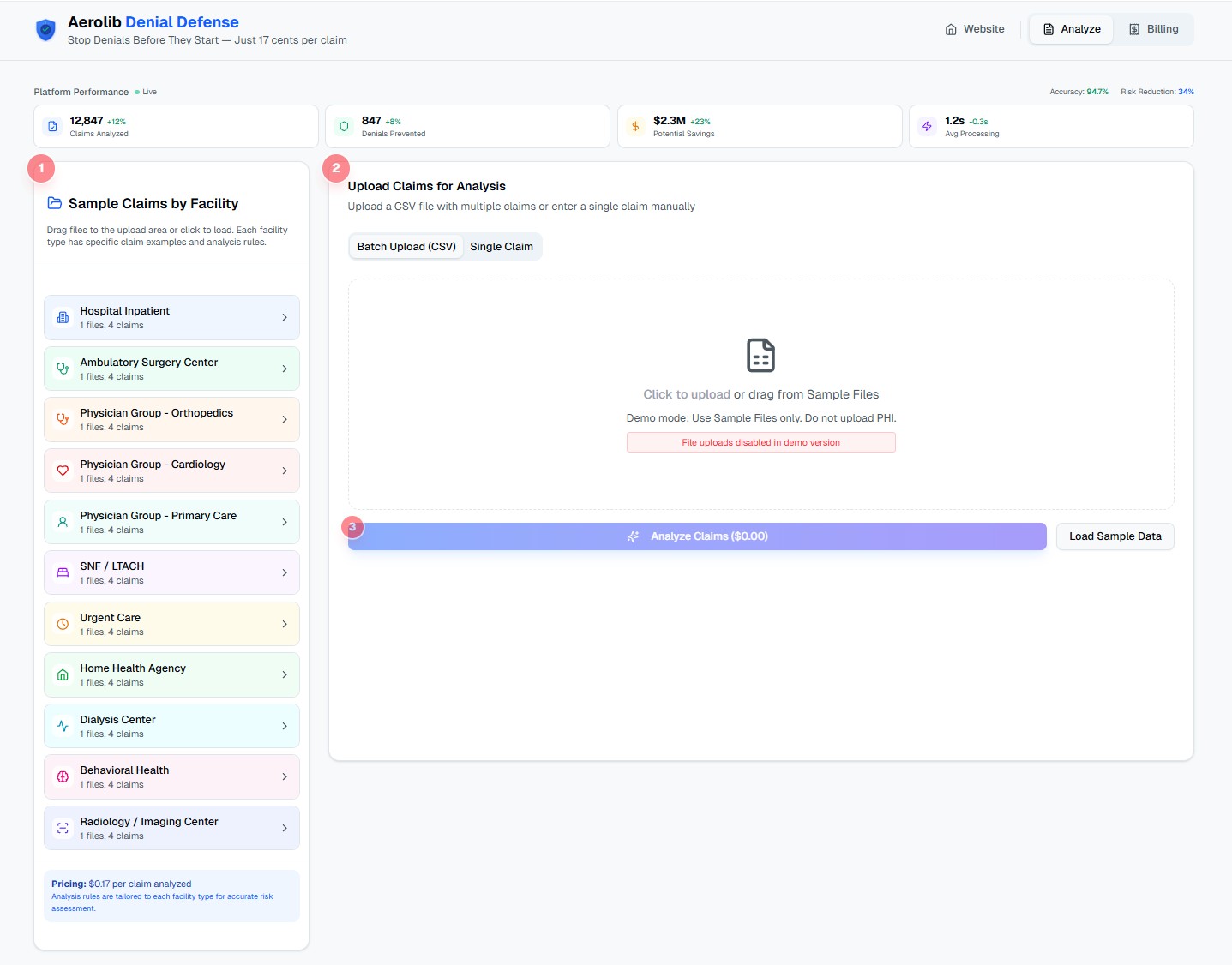
Analyze claims across 11 facility types with real-time performance metrics and facility-specific analysis rules
40%
Denial Rate Reduction
< 2 sec
Analysis Time
$0.17
Per Claim Review
15+
Risk Rules Checked
Tailored Analysis for Every Facility Type
Denial Defense applies specialized denial risk rules for each healthcare setting, ensuring accurate and relevant analysis for your specific facility type.
Hospital Inpatient
DRG validation, LOS analysis, admission criteria
Ambulatory Surgery Center
Procedure appropriateness, site-of-service rules
Physician - Orthopedics
Imaging documentation, surgical necessity
Physician - Cardiology
Test indications, device implant criteria
Physician - Primary Care
Wellness visit documentation, CCM time
SNF / LTACH
Qualifying stays, skilled service requirements
Urgent Care
E/M level support, site appropriateness
Home Health Agency
Homebound status, skilled care requirements
Dialysis Center
ESRD certification, treatment adequacy
Behavioral Health
Therapy authorization, time documentation
Radiology / Imaging
Advanced imaging auth, clinical indications
More Coming Soon
Rehab, DME, Lab, and more facility types
Comprehensive Pre-Submission Analysis
Our AI-powered engine analyzes every claim against 15+ denial risk rules, catching issues before they become costly rejections.
Medical Necessity Validation
Validates length of stay against DRG expectations and flags documentation gaps that commonly trigger denials. Identifies cases where clinical justification may be questioned.
Coding Accuracy Check
Verifies ICD-10 format, identifies missing secondary diagnoses, ensures procedure codes are complete, and catches common coding errors before submission.
Authorization Verification
Flags high-cost procedures requiring pre-authorization, identifies missing authorization numbers, and alerts on procedures typically requiring prior approval.
Timely Filing Alerts
Monitors claim age against payer-specific filing deadlines. Provides early warnings at 30, 60, and 90 days, and critical alerts as deadlines approach.
Payer-Specific Rules
Applies specialized rules for Medicare, commercial payers, and state Medicaid programs. Customize rule weights based on your experience with each payer.
Risk Scoring & Dashboard
Generates actionable risk scores (0-100) with color-coded severity levels. Dashboard shows risk distribution, payer breakdown, and issue categories.
AI-Powered Insights
Intelligent prioritization of issues, context-aware recommendations, and documentation templates tailored to each diagnosis and finding.
Documentation Templates
Pre-built templates for medical necessity documentation, authorization notes, and discharge criteria. Copy-ready text with placeholders for patient specifics.
Team Collaboration
Assign claims to team members, track remediation status, add notes, and maintain a complete audit trail for compliance and quality assurance.
See Denial Defense in Action
From batch analysis to detailed findings, explore how Denial Defense helps you catch denial risks before submission.
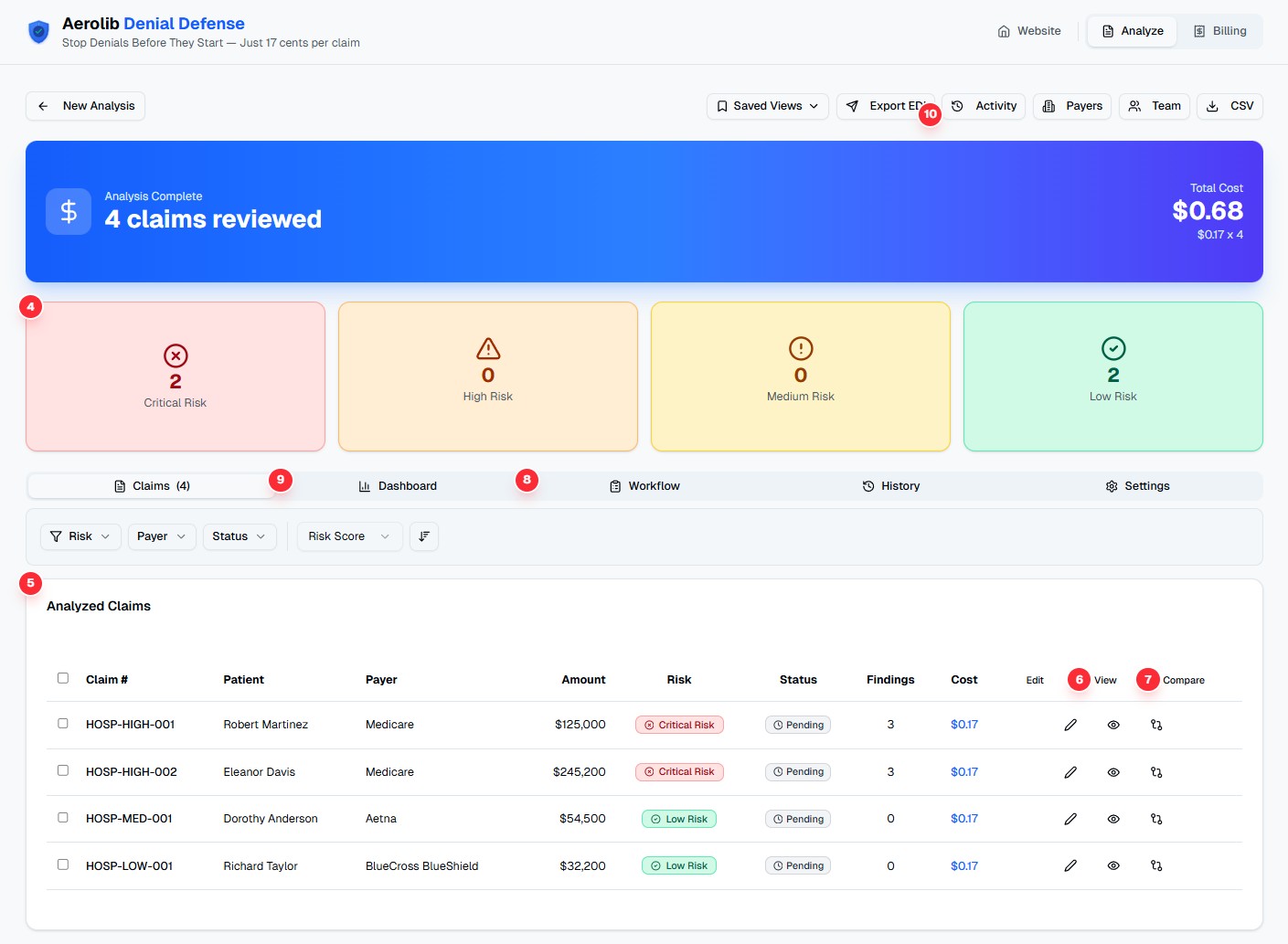
Claims Overview & Risk Summary
See all your analyzed claims at a glance with color-coded risk levels from Critical to Low. Filter by risk level, payer, or status to focus on what needs attention first.
- Color-coded risk cards: Critical (red), High (yellow), Medium (amber), Low (green)
- Sortable claims table with patient, payer, amount, and findings
- Quick status badges showing claim processing state
- One-click access to detailed claim analysis
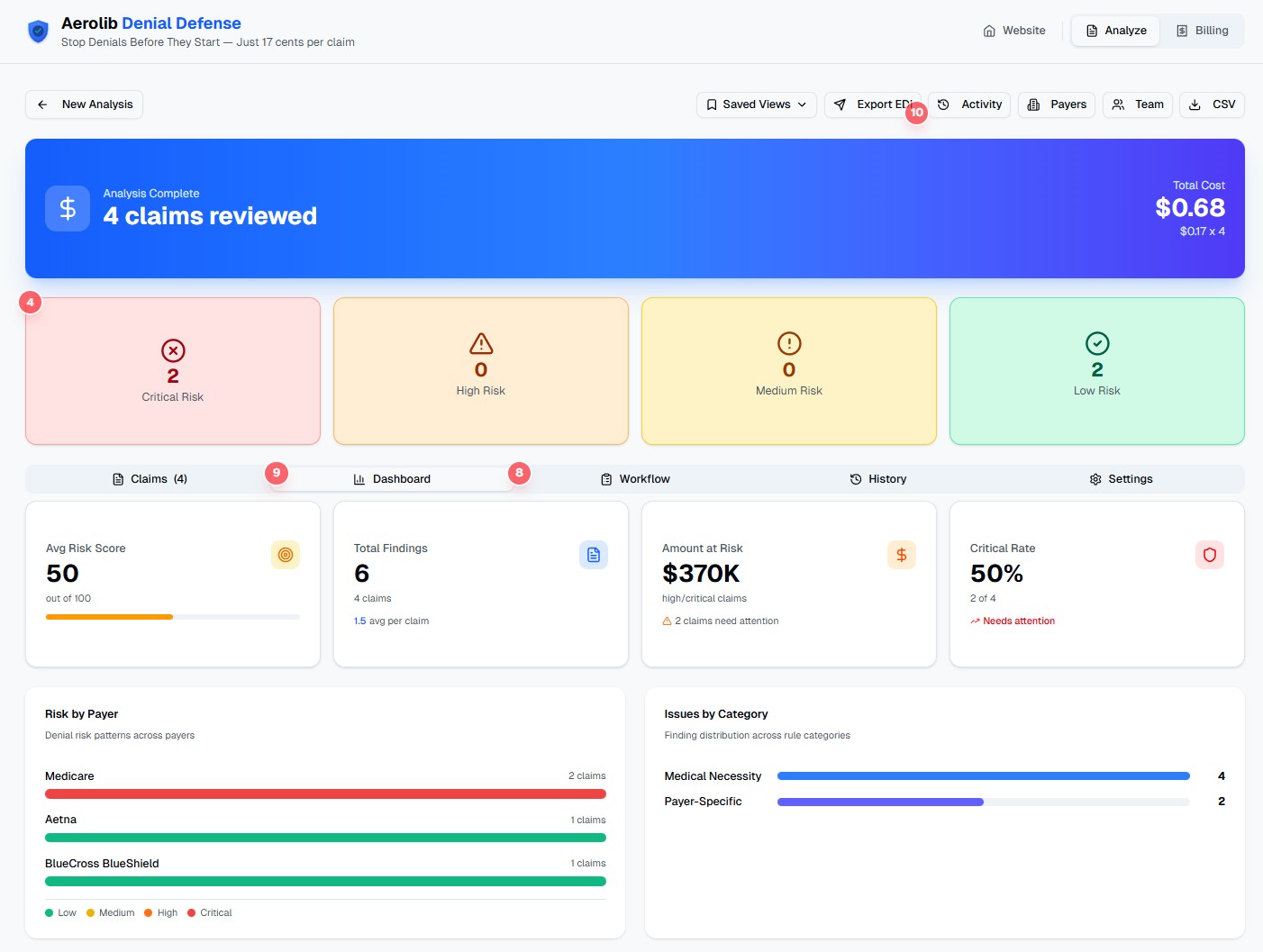
Analytics Dashboard
Get insights into your denial risk patterns with comprehensive analytics. See risk distribution by payer, track issue categories, and identify trends to improve your pre-submission process.
- Average risk score with trend indicators
- Total findings breakdown across all claims
- Amount at risk from high/critical claims
- Risk by payer showing which payers need attention
- Issues by category (Timely Filing, Authorization, Coding, etc.)
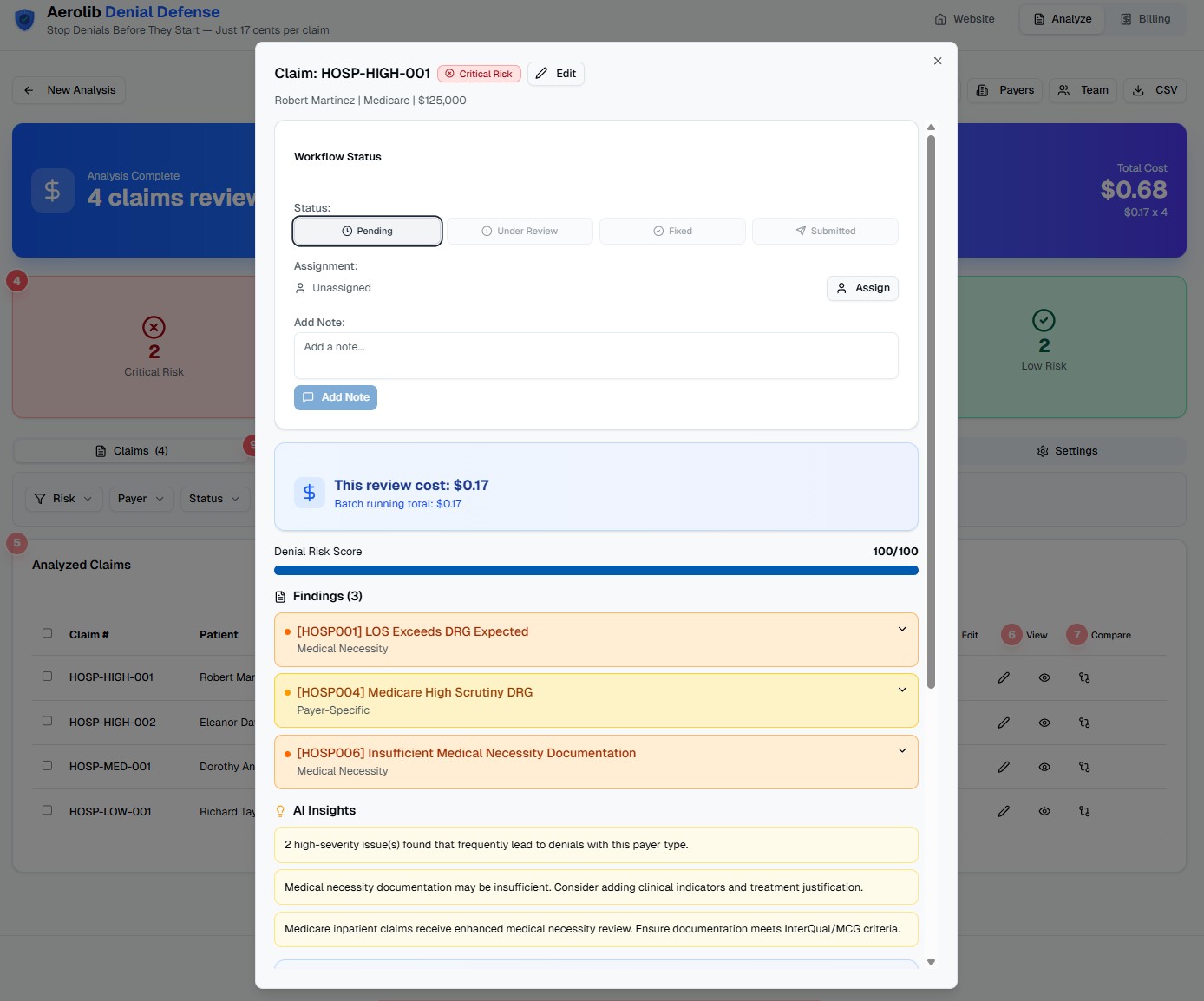
AI-Powered Insights & Templates
Each claim includes AI-generated insights that prioritize issues and provide context-aware recommendations. Documentation templates help you quickly address findings with proper clinical language.
- Specific recommendations based on your findings
- Documentation templates for each diagnosis type
- Copy-ready text with bracketed placeholders
- Expandable findings with detailed explanations
- Severity-coded alerts (urgent, high, warning)
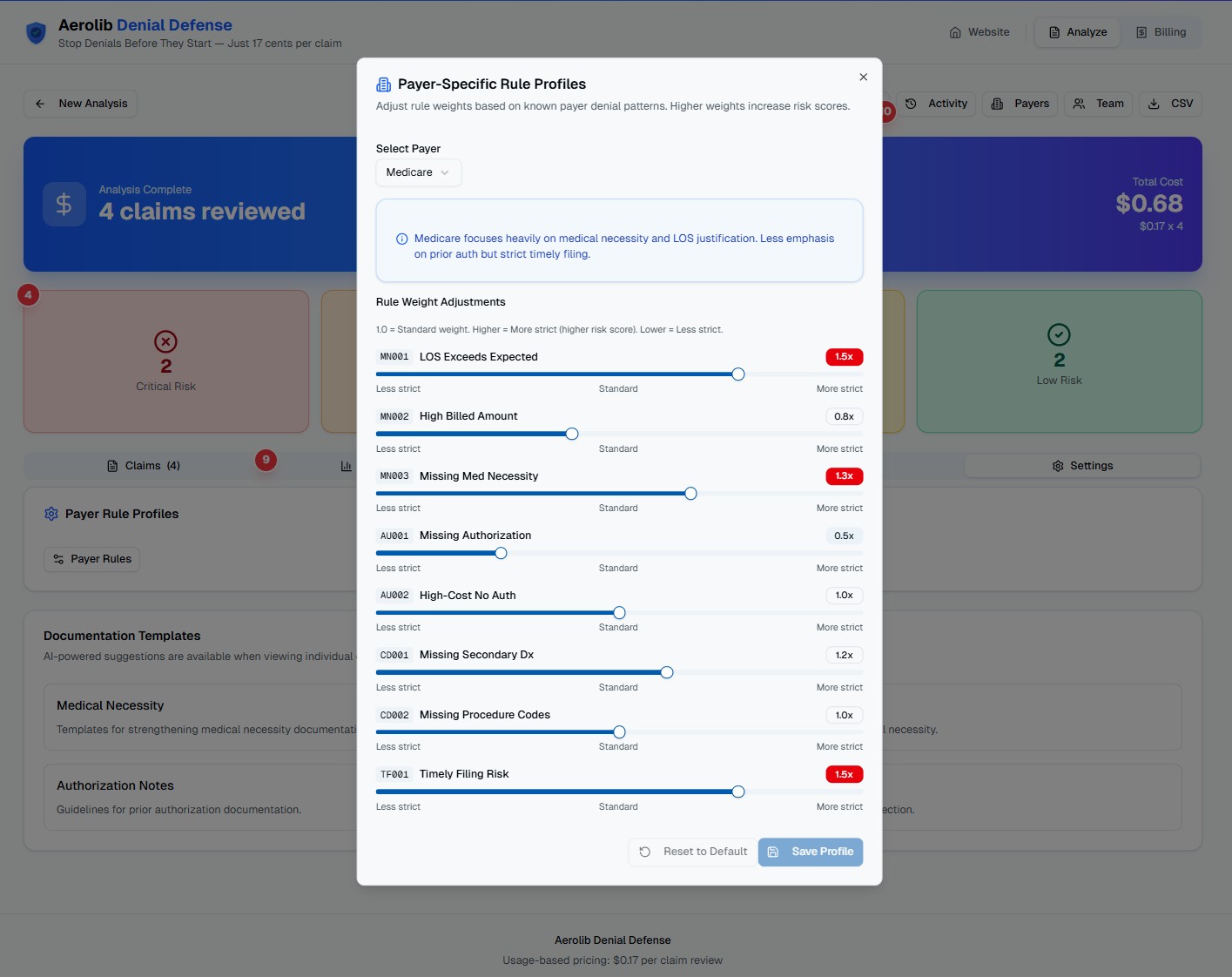
Payer-Specific Rule Profiles
Customize rule weights based on known payer denial patterns. Medicare focuses on medical necessity while commercial payers may emphasize authorization. Tune the analysis to match your experience.
- Pre-configured profiles for Medicare, Medicaid, and major payers
- Adjustable rule weights from 0.5x to 2.0x
- Payer-specific insights and recommendations
- Save custom profiles for your payer mix
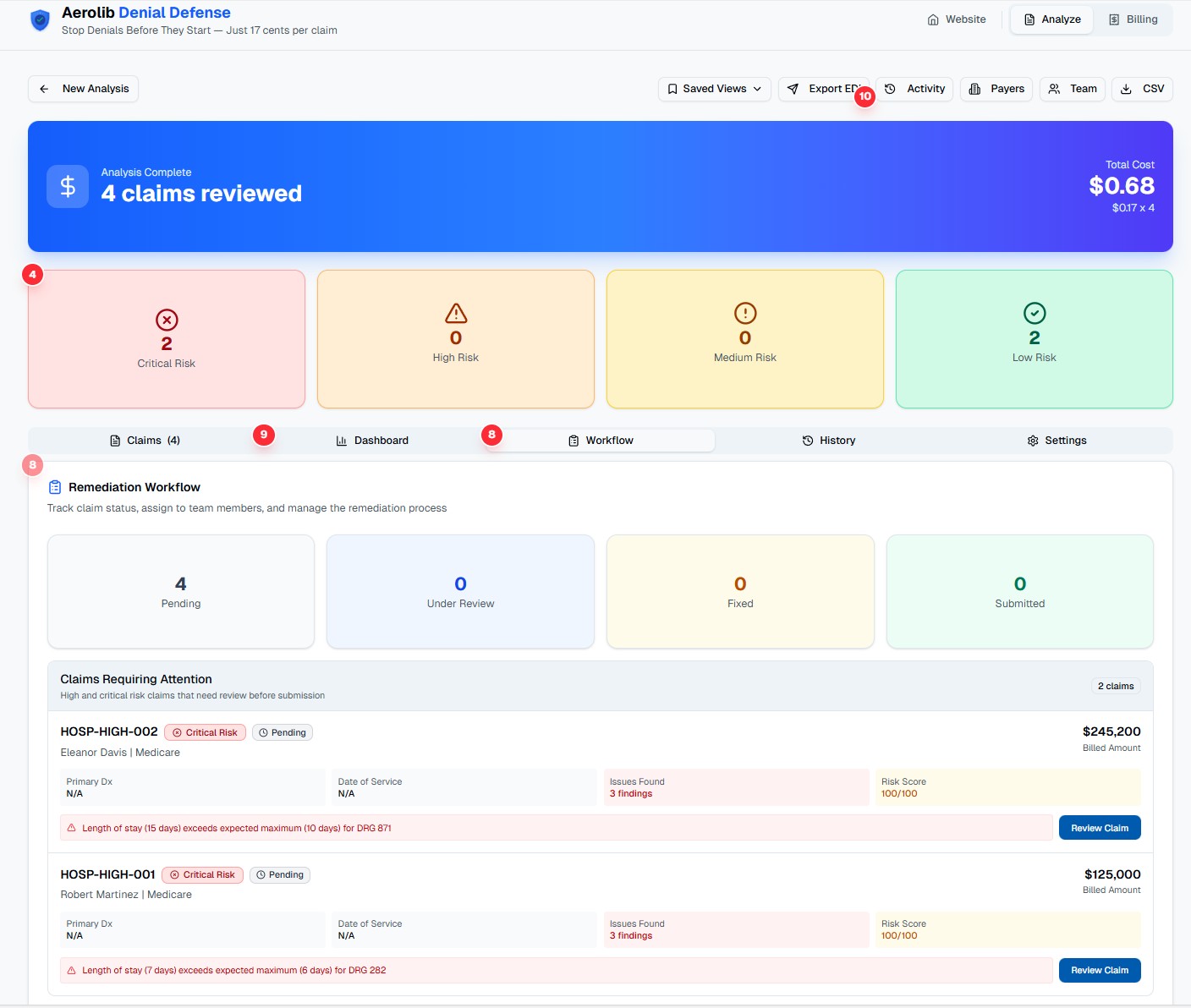
Workflow & Team Management
Track remediation progress across your team. Assign claims to specific team members, update status as work progresses, and see who's working on what at a glance.
- Workflow status: Pending, Under Review, Fixed, Submitted
- Team assignments with workload visibility
- Claims requiring attention queue
- Status-based filtering and prioritization
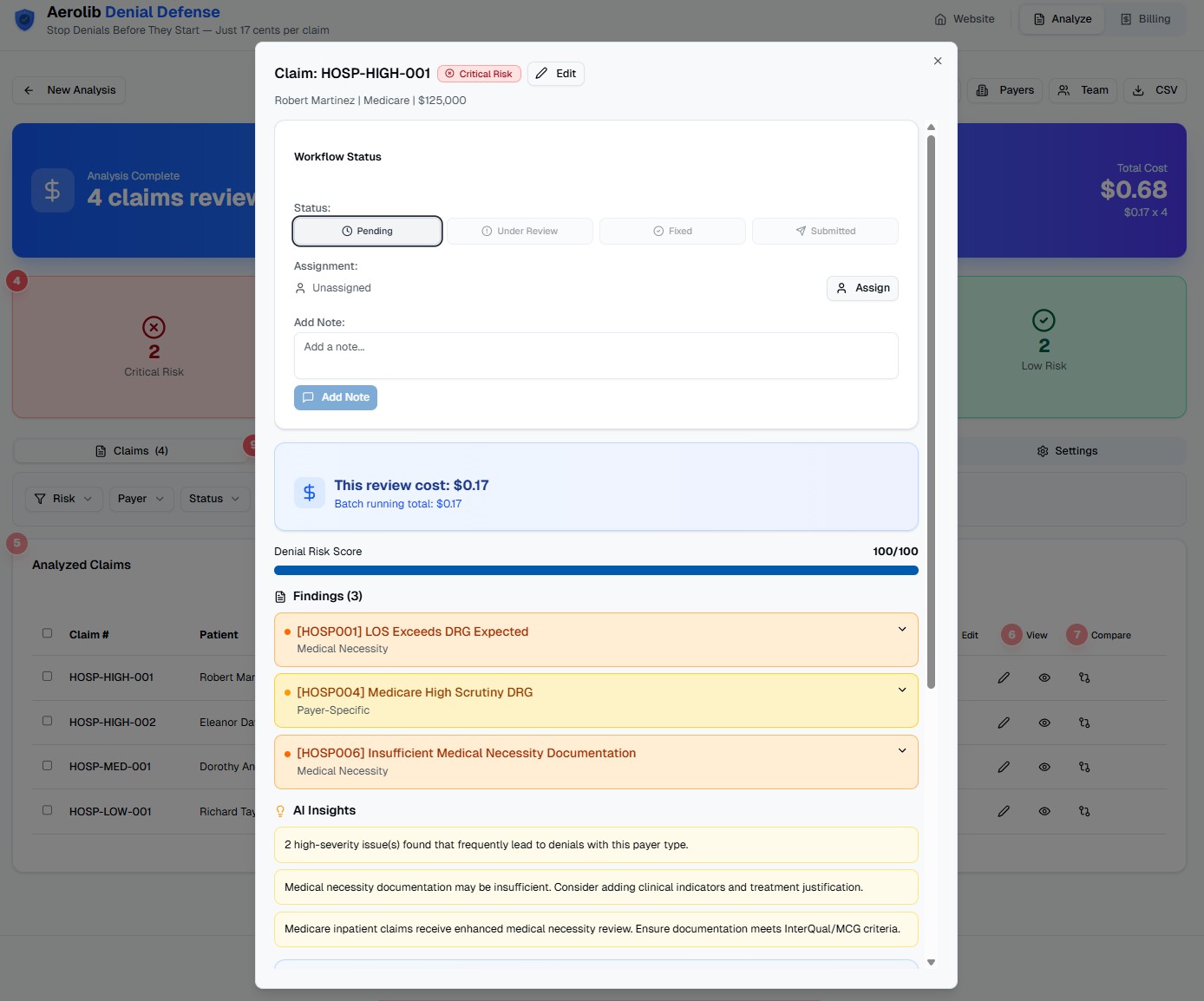
Complete Claim Management
Everything you need to manage a claim in one place. Update workflow status, add notes, track costs, and access AI documentation suggestions all from the claim detail view.
- Per-claim cost tracking ($0.17 per review)
- Denial risk score visualization (0-100)
- AI documentation suggestions with 5+ templates
- Note-taking for team communication
- Assign to team members with one click
How It Works
Get from upload to actionable insights in seconds, not hours.
Upload Claims
Upload a CSV batch or enter individual claims. Supports standard claim formats with automatic field mapping. Use our sample files to get started.
Instant Analysis
Our AI engine runs 15+ denial risk rules in under 2 seconds. Each claim receives a risk score, categorized findings, and specific recommendations.
Review & Export
Review findings, assign to team members, track remediation status, and export clean claims. Export to CSV, PDF, or EDI X12 837 format.
Flexible, Contract-Based Pricing
Customized pricing tailored to your organization's needs.
Platform access fee + per-claim pricing
Starting at $0.17 per claim
Pricing based on:
- • Claim volume commitments
- • Contract duration
- • Number of user seats
- • Facility types & integrations
- • Support level requirements
- Full 15+ rule analysis
- AI-powered insights & recommendations
- Documentation templates
- Risk scoring and dashboards
- Payer-specific rule profiles
- Team collaboration & workflow
- CSV, PDF, and EDI export
- Dedicated support
Frequently Asked Questions
Everything you need to know about Denial Defense.
Ready to Reduce Denials?
Contact us to schedule a demo or get started with Denial Defense.